1Department of Internal Medicine, University of Ioannina Medical School, University Hospital of Ioannina, Ioannina, Greece; 2Department of Internal Medicine, Aristotle University of Thessaloniki Medical School, Hippokration Hospital, Thessaloniki, Greece; 3Department of Cardiology, Tzaneio Hospital, Piraeus, Greece; 4First Department of Pediatrics, National and Kapodistrian University of Athens Medical School, St. Sophia Children Hospital, Athens, Greece; 5Second Department of Pediatrics, Medical School, National & Kapodistrian University of Athens, “P. & A. Kyriakou” Children’s Hospital; 6Department of Cardiology, Onassis Cardiac Surgery Centre, Athens, Greece; 7Department of Internal Medicine, Aristotle University of Thessaloniki Medical School, Papageorgiou Hospital, Thessaloniki, Greece; 8Department of Cardiology, University of Athens Medical School, Attikon University Hospital, Athens, Greece; 9Department of Cardiology, University Hospital of Heraklion, Heraklion, Greece; 10Department of Cardiology, Hippokration Hospital, Athens, Greece; 11First Propedeutic Department of Internal Medicine, Aristotle University of Thessaloniki Medical School, AHEPA Hospital, Thessaloniki, Greece
Familial hypercholesterolemia (FH) is the most common metabolic genetic disorder. It is estimated that around 13 million people worldwide have FH. At the same time, only 25% of FH patients have been diagnosed. Moreover, these patients are often undertreated. The true prevalence of FH in Greece is unknown, but it is estimated that there are at least 40,000 FH patients nationwide pointing to a prevalence of 1:250. Patients with FH are at a high risk for cardiovascular events and death at an early age. Therefore, prompt detection of these patients is of pivotal importance in order to implement appropriate preventive measures at a young age. Patient registries are a powerful tool for recording and monitoring a disease and promoting clinical practices, thus contributing to improved outcomes and reduction of healthcare costs. National registries of FH patients have been a success in the Netherlands, Spain and Wales. As Greece did not have a national FH registry, the Hellenic Atherosclerosis Society has organized, established and funded the Hellenic Familial Hypercholesterolemia (HELLAS-FH) national registry in order to promote a better understanding of FH in our country.
Familial hypercholesterolemia, Greece, Hellenic Familial Hypercholesterolemia Registry, Registry
INTRODUCTION
Hyperlipidemia is one of the key risk factors for the development of cardiovascular disease (CVD). Among the various causes of hyperlipidemia, familial hypercholesterolemia (FH) is both common as well as underdiagnosed.1 FH is an autosomal dominant genetic disease2 with an estimated number of patients of around 13 million worldwide.3 The FH-associated lipid disorder is mainly attributed to mutations of the low-density lipoprotein (LDL) receptor gene, which lead to impaired functionality or decreased synthesis of the LDL receptor. As a result, decreased clearance of plasma LDL cholesterol (LDL-C) is observed.2 The resulting marked hyperlipidemia coupled with an onset very early in life is associated with development of atherosclerosis and higher CVD risk of affected patients.4-7 Moreover, FH subjects beyond being underdiagnosed are also frequently undertreated.8-11 It follows that increased awareness of the disease is very important and required for an early diagnosis to be established and an aggressive management of FH patients to be applied.12 According to the latest data, the incidence of FH heterozygotes in the general population is 1:250, while in certain areas this can be as high as 1:100.13,14 In Greece, it is estimated that there are at least 40,000 FH patients, but the true prevalence is unknown.
HELLAS-FH REGISTRY: RATIONALE
The Hellenic Atherosclerosis Society (a non-profit scientific organization) has established the Hellenic Familial Hypercholesterolemia (HELLAS-FH) Registry as a national, multi-center initiative to identify FH patients in Greece, track treatment and record clinical outcomes over time. A number of sites (Table 1) have been selected to enroll FH patients in a national database and record baseline and annual follow-up laboratory and clinical data as well as document clinical events. In the context of HELLAS-FH, systematic screening strategies such as cascade screening will be utilized in order to improve identification of FH patients. Cascade screening provides a cost-effective way of identifying new cases of FH. Using this method, a person diagnosed with FH, referred to as the index case, becomes the starting point in their family tree from where a systemic screening of first degree relatives is implemented.
Most FH patients are diagnosed based on clinical and biochemical criteria: a) early history of coronary heart disease (in terms of personal history or in 1st degree relatives) and b) levels of LDL-C >95th percentile for age and sex.13 The tendinous xanthomata, often localized on the Achilles tendon and/or the extensor tendons of the upper limbs, are almost pathognomonic of FH but not necessary for the diagnosis.13 The presence of early arcus cornealis (at age <45 years) and xanthelasmata are common in these patients and suggest an inherited lipid disorder.13 Genetic testing of subjects can also be used to identify FH patients. However, genetic testing has some limitations. Indeed, depending on the laboratory’s capacity, genetic testing can screen only for limited known gene mutations associated with FH. As a result, mutations not yet discovered to be linked with FH will be missed. Moreover, the considerable economic cost of gene testing constitutes another hindrance to the wide implementation of this process as a screening method. Consequently, several sets of diagnostic criteria for FH are in clinical use, such as MED-PED (Make Early Diagnosis-Prevent Early Death) criteria in the United States,15 the Simon Broome Register criteria in the United Kingdom16 and the Dutch Lipid Clinic Network criteria in the Netherlands.13,16,17 As mentioned above, FH is often underdiagnosed and its prevalence is underestimated.4 One reason behind these shortcomings is insufficient training among healthcare professionals as well as lack of awareness among health policy-makers and the general public regarding FH.18
As previously discussed, FH is associated with a high risk of premature CVD events and death. Therefore, it is imperative that FH patients be diagnosed early and appropriate treatment strategies be promptly implemented. An aggressive management plan is expected to decrease CVD risk in these patients. Indeed, statin treated FH patients have a similar risk of coronary heart disease compared with the general population.12
Treatment of FH patients is based on the combination of dietary interventions together with lifelong hypolipidemic pharmacotherapy. The target is to decrease LDL-C levels by at least 50% and reach LDL-C levels <100 mg/dL in adults without CVD and <130 mg/dL in children.6,13,19-21 Statin treatment is the cornerstone of FH management, while ezetimibe and colesevelam are supplementary options.13 Recently, novel drugs such as proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors have been added to the available management strategies of specific patient subgroups.22,23 Individuals who exhibit statin intolerance or cannot achieve treatment targets should be referred to specialized clinics.13
The knowledge which the HELLAS-FH registry will provide can lead to better understanding of the true prevalence of FH in Greece. Moreover, the registry will provide evidence-based data regarding FH, which will give a new insight into the disease and promote a more aggressive and thus effective management. In addition, by increasing the awareness of public healthcare policy-makers regarding FH prevalence, it will contribute to the implementation of enhanced healthcare plans in order to customize and improve the care of these patients
HELLAS-FH REGISTRY: AIMS
The aim of this study is to create a national online registry of patients with FH targeting the following primary goals: a) to diagnose, treat and educate people with FH and b) to further spread information about this disease to medical practitioners, other healthcare professionals, policy-makers and the general public. The collected data will help make them more aware of the actual FH burden. As a result, it is expected that physicians will be more vigilant regarding the diagnosis and management of FH and promote cascade screening. In addition, genetic testing should be encouraged and offered as an option to more subjects when a diagnosis of FH is possible. However, for extended genetic testing of subjects to become a viable option, a considerable decrease of the associated economic costs is required. One option that could contribute to this, would be the establishment of only a couple of central genetic testing facilities in Greece that would handle samples from all over the country.
Furthermore, HELLAS-FH registry will gather accurate data regarding: a) the prevalence of FH, b) the current FH management strategies, c) the prevalence of clinical outcomes in FH patients and d) the common obstacles, pitfalls and mistakes in the successful management of FH. Finally, the registry can stimulate a scientific collaboration amongst researchers in order to further promote systematic FH investigation and understanding. The HELLAS-FH registry is part of the FH Studies Collaboration (FHSC) sponsored by the European Atherosclerosis Society (EAS).24
HELLAS-FH REGISTRY: METHODS
Inclusion/Exclusion Criteria
All patients with baseline LDL-C levels >190 mg/dL (adults) or >160 mg/dL (children) will be evaluated in accordance with the Dutch Lipid Clinic Network criteria. Of note, there is an 85% agreement rate between these criteria and genetic diagnosis of the disease.25 Before the inclusion of patients in the registry, a preliminary evaluation regarding their eligibility will be conducted (Figure 1). To be included in the registry, patients will need to meet all the inclusion criteria and none of the exclusion criteria:
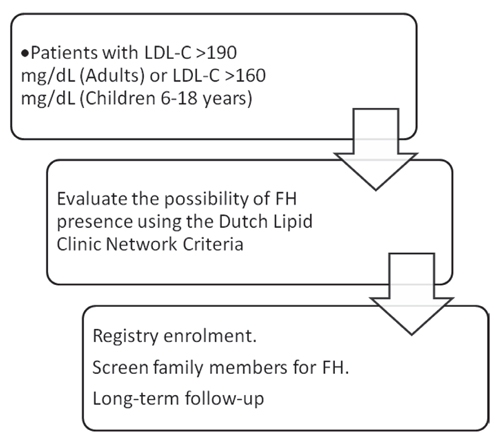
Figure 1. Flowchart of the patient screening process for registry enrollment.
Inclusion criteria:
Children (6-18 years) with LDL-C >160 mg/dL and adults (>18 years) with LDL-C >190 mg/dL and a clinical diagnosis of FH according to the Dutch Lipid Clinic Network Criteria.
Willingness to participate to the study and sign the informed consent form (ICF).
Exclusion criteria:
Any clinically significant disorder recognized at the time of the preliminary assessment which, at the discretion of the investigator, would exclude the safe completion of the study or limit the assessment of endpoints (e.g. major systemic diseases, patients with short life expectancy).
Registry captured data
HELLAS-FH registry will record a series of variables related to FH in two steps. The first step will include the initial recording of a new patient in the registry, while the second step will include the per year update of patient data. The purpose of the registry is to create a continuous, dynamic data collection relating to the condition of the patient, the disease course and outcomes in conjunction with administered treatments.
The sources for data recorded in the registry will be patient’s medical history, family history and medical records, patient lab tests and imaging studies as well as any findings from the physical examination such as weight, height, waist circumference, blood pressure as well as the presence of corneal arcus, xanthomata or xanthelasmata. During the initial recording of a patient, the data presented in Table 2 will be recorded. After signing the ICF, patients will acquire printed information about the HELLAS-FH registry in order to better educate themselves about FH as well as encourage other members of their family to contact the clinic for further evaluation in the context of cascade screening. In cases where genetic analysis is available from the patient’s history, this will allow the definitive diagnosis of FH and will also help the identification of new mutations. Currently, in Greece there are two public genetic laboratories for testing mutations related with FH: 1. The Laboratory of Medical Genetics in Clinical Practice located in Ioannina, which is associated with the University of Ioannina, and 2. The Medical Genetics Laboratory located in the Choremio Research Laboratory in St. Sophia Children’s Hospital in Athens, which is associated with the National and Kapodistrian University of Athens.
Demographic data concerning the professional status will be collected (based on the US Standard Occupational Classification and the UK Standard Occupational Classification).26,27 In addition, the educational level of patients will be recorded according to the “International Standard Classification of Education, ISCED 2011”, UNESCO Institute of Statistics.28 Patients will be reevaluated once a year during their long-term monitoring (Table 2).
DATA MANAGEMENT
A number of specialized lipid clinics in Greece were invited to participate in the HELLAS-FH registry (Table 1). Prior to entering patient data into the registry, each site will be required to receive Institutional Review Board (IRB) approval and obtain patient informed consent. For patients aged 6-18 years, patient informed assent as well as informed consent of parents/guardians will be required. The registry will be conducted in accordance with the principles of the Declaration of Helsinki, as well as in accordance with the laws and regulations that govern ethical management of patients voluntarily participating in non-interventional studies.
Registry data will be collected and posted through a secure online portal per center. This means that each investigator will be able to enter, access and modify patient data relating only to his/her site. Investigators will enter data in an electronic case report form consisting of two interfaces. The first will involve patient identification by his unique national insurance number and the second the entry/update of the registry data. This procedure is necessary to avoid creating duplicates in the registry and to preserve the anonymity of each patient. During patient entry, the system will generate a unique registry code number, which will be connected with the patient’s national insurance number. This code will be the connection between patient identification and medical data in the registry (Figure 2). HELLAS-FH registry has been approved by the Hellenic data protection authority.

Figure 2.
Data management and preservation of anonymity of medical data
CONCLUSIONS
The HELLAS-FH registry is the first nationwide FH registry in Greece which will hopefully provide important evidence regarding the management of FH patients in our country. Registries can significantly improve the management of a medical condition by providing better insight into the problem while allowing for comparison of results with larger reference populations. Registry results may stimulate improvements in quality and consistency of clinical practice and guide the establishment of a national policy for the diagnosis and treatment of FH.
CONFLICTS OF INTEREST STATEMENT
CVR, AG and GC have no relevant conflict of interest to report. VA has an association with the pharmaceutical companies Amgen, Sanofi, MSD, Mylan and Lilly. KT has participated in educational, research and advisory activities sponsored by Amgen, Angelini, Astra-Zeneca, Bayer, Boehringer-Ingelheim, Elpen, Lilly, MSD, Mylan, Novo Nordisk, Sanofi and Vianex. GK has given talks, attended conferences and participated in trials sponsored by Amgen, Angelini, MSD, Lilly, Vianex and Sanofi-Aventis and has also accepted travel support to conferences from Amgen, Sanofi and MSD. EB has received honoraria, clinical trials, consultant fees from MSD and Sanofi-Aventis. VK has given talks and attended conferences sponsored by AstraZeneca, MSD, Sanofi-Aventis and Vianex. ES has participated in educational and advisory activities sponsored by Astra-Zeneca, Medtronic, MSD, Sanofi and Servier. LR has received honoraria for lectures, clinical trials and consultant fees from Amgen, MSD, AstraZeneca, Sanofi-Aventis and Pfizer. IS has given talks, received honoraria and participated in clinical trials sponsored by MSD, Amgen, Sanofi. ENL has participated in educational, research and advisory activities sponsored by Astra-Zeneca, MSD, Lilly, Bayer, Amgen, Sanofi, Boehringer-Ingelheim, Novartis, Novo Nordisk and Servier.
FUNDING
This study is funded by the Hellenic Atherosclerosis Society from grants provided by Amgen, Sanofi, MSD and Eli-Lilly.
REFERENCES
1. Neil HA, Hammond T, Huxley R, Matthews DR, Humphries SE, 2000 Extent of underdiagnosis of familial hypercholesterolaemia in routine practice: prospective registry study. BMJ 321: 148.
2. Brautbar A, Leary E, Rasmussen K, et al, 2015 Genetics of familial hypercholesterolemia. Curr Atheroscler Rep 17: 491.
3. Ned RM and Sijbrands EJ, 2011 Cascade Screening for Familial Hypercholesterolemia (FH). PLoS Curr 3: RRN1238.
4. Nordestgaard BG, Chapman MJ, Humphries SE, et al, 2013 Familial hypercholesterolaemia is underdiagnosed and undertreated in the general population: guidance for clinicians to prevent coronary heart disease: consensus statement of the European Atherosclerosis Society. Eur Heart J 34: 3478-3490a.
5. Cuchel M, Bruckert E, Ginsberg HN, et al, 2014 Homozygous familial hypercholesterolaemia: new insights and guidance for clinicians to improve detection and clinical management. A position paper from the Consensus Panel on Familial Hypercholesterolaemia of the European Atherosclerosis Society. Eur Heart J 35: 2146-2157.
6. Wiegman A, Gidding SS, Watts GF, et al, 2015 Familial hypercholesterolaemia in children and adolescents: gaining decades of life by optimizing detection and treatment. Eur Heart J 36: 2425-2437.
7. Hopkins PN, Toth PP, Ballantyne CM, Rader DJ, National Lipid Association Expert Panel on Familial H, 2011 Familial hypercholesterolemias: prevalence, genetics, diagnosis and screening recommendations from the National Lipid Association Expert Panel on Familial Hypercholesterolemia. J Clin Lipidol 5: Suppl 3: 9-17.
8. Benn M, Watts GF, Tybjaerg-Hansen A, Nordestgaard BG, 2012 Familial hypercholesterolemia in the danish general population: prevalence, coronary artery disease, and cholesterol-lowering medication. J Clin Endocrinol Metab 97: 3956-3964.
9. Pijlman AH, Huijgen R, Verhagen SN, et al, 2010 Evaluation of cholesterol lowering treatment of patients with familial hypercholesterolemia: a large cross-sectional study in The Netherlands. Atherosclerosis 209: 189-194.
10. Rizos CV, Barkas F, Elisaf MS, 2014 Reaching low density lipoprotein cholesterol targets. Curr Med Res Opin 30: 1967-1969.
11. Barkas F, Liberopoulos E, Liamis G, Elisaf M, 2016 Familial hypercholesterolemia is undertreated in clinical practice. Hellenic J Atheroscler 7: 120-130.
12. Versmissen J, Oosterveer DM, Yazdanpanah M, et al, 2008 Efficacy of statins in familial hypercholesterolaemia: a long term cohort study. BMJ 337: a2423.
13. Goldberg AC, Hopkins PN, Toth PP, et al, 2011 Familial hypercholesterolemia: screening, diagnosis and management of pediatric and adult patients: clinical guidance from the National Lipid Association Expert Panel on Familial Hypercholesterolemia. J Clin Lipidol 5:Suppl 3: 1-8.
14. Yuan G, Wang J, Hegele RA, 2006 Heterozygous familial hypercholesterolemia: an underrecognized cause of early cardiovascular disease. CMAJ 174: 1124-1129.
15. Williams RR, Hunt SC, Schumacher MC, et al, 1993 Diagnosing heterozygous familial hypercholesterolemia using new practical criteria validated by molecular genetics. Am J Cardiol 72: 171-176.
16. Scientific Steering Committee on behalf of the Simon Broome Register Group, 1991 Risk of fatal coronary heart disease in familial hypercholesterolaemia. Scientific Steering Committee on behalf of the Simon Broome Register Group. BMJ 303: 893-896.
17. D’Agostino RB, Vasan RS, Pencina MJ, et al, 2008 General cardiovascular risk profile for use in primary care: the Framingham Heart Study. Circulation 117: 743-753.
18. Vallejo-Vaz AJ, Kondapally Seshasai SR, Cole D, et al, 2015 Familial hypercholesterolaemia: A global call to arms. Atherosclerosis 243: 257-259.
19. Elisaf M, Pitsavos C, Liberopoulos E, Tziomalos K, Athyros V, 2014 Updated guidelines of the Hellenic Society of Atherosclerosis for the diagnosis and treatment of dyslipidemia-2014 Hellenic J Atheroscler 5: 161-163.
20. Catapano AL, Graham I, De Backer G, et al, 2016 2016 ESC/EAS Guidelines for the Management of Dyslipidaemias. Eur Heart J 37: 2999-3058.
21. Descamps OS, Tenoutasse S, Stephenne X, et al, 2011 Management of familial hypercholesterolemia in children and young adults: consensus paper developed by a panel of lipidologists, cardiologists, paediatricians, nutritionists, gastroenterologists, general practitioners and a patient organization. Atherosclerosis 218: 272-280.
22. Chapman MJ, Stock JK, Ginsberg HN, Forum P, 2015 PCSK9 inhibitors and cardiovascular disease: heralding a new therapeutic era. Curr Opin Lipidol 26: 511-520.
23. Achimastos A, Alexandrides T, Alexopoulos D, et al, 2016 Expert consensus on the rational clinical use of proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors. Hormones (Athens) 15: 8-14.
24. Vallejo-Vaz AJ, Akram A, Kondapally Seshasai SR, et al, 2016 Pooling and expanding registries of familial hypercholesterolaemia to assess gaps in care and improve disease management and outcomes: Rationale and design of the global EAS Familial Hypercholesterolaemia Studies Collaboration. Atheroscler Suppl 22: 1-32.
25. Civeira F, Ros E, Jarauta E, et al, 2008 Comparison of genetic versus clinical diagnosis in familial hypercholesterolemia. Am J Cardiol 102: 1187-1193.
26. Bureau of Labor Statistics. The 2010 Standard Occupational Classification. 2010; Available from: https://www.bls.gov/soc/soc_2010_user_guide.pdf.
27. Office for National Statistics. The current standard occupational classification for the UK. 2010; Available from: https://www.ons.gov.uk/methodology/classificationsandstandards/standardoccupationalclassificationsoc/soc2010.
28. International Standard Classification of Education, ISCED 2011. 2011; Available from: http://uis.unesco.org/sites/default/files/documents/international-standard-classification-of-education-isced-2011-en.pdf.
Address for correspondence:
Dr Evangelos Liberopoulos, MD, FASA, FRSH, Associate Professor of Internal Medicine, Department of Internal Medicine, Medical School, University of Ioannina, Ioannina 45110, Greece; Tel.: +30-26510-07502, Fax: +30-26510-07016, E-mail: elibero@cc.uoi.gr
Received: 25-07-2017, Accepted: 05-11-2017